|
Home : Quarterly Archives : Volume 26 |
Tredyffrin Easttown Historical Society |
|
Source: July 1988 Volume 26 Number 3, Pages 90–104 Medicine in the Revolutionary War
I. State of the Art and its Practitioners To appreciate fully the practice of medicine in the Revolutionary War, the state of health and disease control, and the medical practioners in the colonies during the latter part of the 18th century, must first be considered. Life expectancy was only thirty-five years. There was a universal ignorance of the principles of contagion and sanitation. Polluted earth and marsh gases were felt to be the prime factor. Lice flourished as bathing was considered by many to be dangerous. Epidemics were for the most part unchecked, and regular ravages of diseases such as smallpox, typhus, yellow fever and a variety of other fevers, measles, and dyentery (flux) abounded. Most families lost numbers of children to disease; grim evidence of this can be found in old cemeteries throughout the area. Because of woefully inadequate conditions, there was a high mortality rate in pregnancies and deliveries, where only relatives and midwives were available. It was rare to find an adult with a full set of teeth. Dental extractions and the setting of broken bones were performed by whomever was available. Interesting, the Quakers were locally considered by outsiders to be a healthier breed than average, and were noted for their longevity. The chief medical figure was the housewife, of whom there was no shortage. She, armed with a stock of superstitions, folk remedies, family tales, and home-grown herbs, cared for her family and neighbors. In addition, she might have access to newspapers, almanacs, and medical handbooks. A variety of British patent medicines were available in country stores, as well as local concoctions. During the war, privateers were to provide British medicines, which were supplemented by ingenious American counterfeiters. Because of the uncertain state of medicine, numerous "quacks" were to be found, and undoubtedly provided at least emotional support. Smaller communities were served medically by the clergymen and the better educated farmers. By 1776, 3000 to 4000 individual practitioners of medicine were available in the colonies, of which 300 to 400, largely located in urban areas, had medical degrees. Most of the physicians with degrees were graduates of Edinburgh College, the model for the first two medical schools to be established in America during the colonial period. Philadelphia was better supplied with physicians than any other town. Between 1740 and 1775, 82% of them had studied in Europe, and most of them had degrees. The supply of physicians in Pennsylvania was comparable to that of provinical England, and a surprising number were in country towns. The cost of such care was not inexpensive, but even members of the laboring class could afford it. Most physicians earned £100 to £200 annually, and were able to accumulate £500 worth of property. Some doctors served the poor for token payments, and charged the rich with high fees --along-standing English custom, and one which has continued into recent years. A benevolent gesture were the Pennsylvania fund-raising drives to finance smallpox inoculation of the poor, a program which actually was beneficial for all.. None of the physicians - even the 300 to 400 with degrees--was licensed, as licensing procedures existed only in Europe. In 1772 New Jersey passed a law establishing licensure examinations, to be conducted by the Supreme Court of the state, but it was never fully implemented. During the colonial period, two medical schools were established in the colonies - the Medical Department of the College of Philadelphia (later the University of Pennsylvania) in 1765, and The Kings College (later Columbia University) in New York City in 1768. By 1776 only 51 degrees had been conferred by these schools, and then classes were suspended because of the war. The Medical College of Philadelphia was founded by two prominent physicians, John Korgan and William Shippen. (Both these men assumed important roles in the war, but they became adversaries in the process.) Before this, the qualification of a medical student was based on an intensive apprenticeship of at least five years with a reputable physician. The school course was of two years duration, running from November to June of each year. The first year consisted of pre-clinical subjects - liberal arts with mathematics, natural history, a working knowledge of Latin, and preferrably French as well. The second year included anatomy, materia medica, botany, chemistry, physics, pathology, and clinical medicine. Instruction was by lectures, demonstrations, and attendance upon patients in the Pennsylvania Hospital. At the end of the second year an examination for a bachelor's medical degree was given. This was followed by an additional three years of study and practice, culminating in a stiffer examination that had to be written in Latin, and a thesis which had to be defended before the faculty. But as indicated previously, the vast bulk of the practicing physicians were trained solely by the apprentice system, and they were accorded the same privileges as those who were college-trained. They were almost universal in New England, and the founder of the Harvard Medical College, John Warren, came from their ranks. According to Dr. Banjamin Rush, the only prerequisite for a "doctor's boy" was the ability to stand the sight of blood. After their apprenticeship to a physician, they received a certificate of proficiency and could practice medicine. Their strength was in the development of a practical bedside approach, under the eye of a father-figure. In cities such as Boston, New York, and Philadelphia, they were permitted to sit in on medical lectures. An added element of training for physicians was the use of cadavers for dissection, even as now. However, at that time they were snatched from graves -- usually criminals or paupers, and on occasion a soldier, which led to stern disapproval from General Washington. These bodies were secured at night in cemetery forays, and those involved were known as "nocturnal resurrectionists". Wax models also became popular in Boston, and were even observed by John Adams. An emerging profession in colonial America were druggists and apothecary entrepreneurs. The druggists were only in the largest cities, and prepared drugs for physicians. Apothecaries were far more numerous and were to be found in large towns as well. Often the owners were physicians, and if the establishment was large enough they might employ chemists to prepare the prescriptions. These shops were identified by signs which often featured the "pestle and mortar". The first written prescription was just prior to the Revolutionary War, written by Abraham Chovet, a physician in Philadelphia. In addition to prescription items, over-the-counter preparations -- secret remedies sometimes known as a "sovereign remedy" or a "sure specific" -- were sold. Even at that time, as in the present, concern was voiced about physician-owned apothecaries. Dr. John Morgan felt that the combination of physician and apothecary was not in the best interest of curing patients. TopII. Hospitals Hospitals first appeared in America early in the 18th century. They were hastily built to confine contagious diseases during epidemics, primarily in seaport towns such as New York City, Philadelphia, Newport, Rhode Island, and Charleston, South Carolina. Later in the 18th century the almshouse was established. It was solely for the city's poor, as the better financially-situated chose to be treated in their homes. These almshouses were the first institutions to provide continuous care, and were organized as acts of charity by individuals and sometimes local governmental bodies. The upkeep rested with the local governments. They served a multitude of functions -- for the destitute sick, as orphanages, for criminal incarceration, and for confinement of the insane. The first was in Philadelphia and was organized by William Penn in 1713, originally for destitute Quakers. The next step was the voluntary hospital, a necessity for the growing urbanized middle class, which demanded better care than the almshouses. They generally were begun with philanthropic gifts, but the ongoing operations were financed by voluntary contributions and patients' fees. The first such hospital was the Pennsylvania Hospital, founded in 1751 by Dr. Thomas Bond for the "inhabitation of strangers". As mentioned earlier, it was also helpful in the training of physicians from the Medical College of Philadelphia. However, the New York Hospital, founded in that city in 1775, was the first American hospital to give systematized instruction to medical students. TopIII. Medical Literature At the onset of the Revolutionary War, medical literature in America consisted of one medical book, by the professor of surgery at The Kings College, on the treatment of wounds and fractures; three reprints, and about twenty pamphlets. In short, there was a dearth of printed information. TopIV. Medical Theories and Practices The foundation of colonial medical theory was the Grecian theory of Humors, based on bodily fluids - blood, phlegm, black bile, and yellow bile -which must remain in balance for good health. An excess or deficiency of any one would lead to disease. An excess was relieved by bleeding, purging, and sweating. A deficit was made up by rest, diets, and medicinals. In the 17th century the Humor theory was replaced by one of acidity, alkalinity, saltiness, tension, and relaxation. This was followed in the 18th century by a concept of Nerve Irritation which could alter the body fluids to cause illness. This led to a massive and complex classification of diseases. Symptoms were matched to a text to achieve a diagnosis.
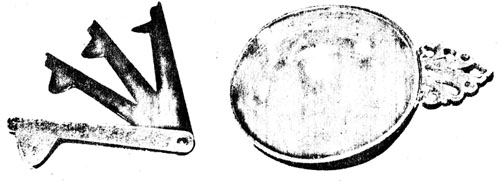
Lancet and bleeding bowl of type used in blood-letting Then a Unity theory was proposed by a Scotsman, John Brown, who felt that good health depended upon a proper balance of nerve stimulation to the muscles, and blood vessel response. Excessive stimulation triggered muscular spasm, which led to disease. Too little stimulation resulted in weakness or atony. This theory prevailed at the time of the Revolution. Excessive irritability was treated by blood-letting, as much as a quart every 48 hours [Note 1] ; by blistering, a counter-irritant of plasters of flannel coated with caustics, such as masked green beetle or Spanish fly; the use of poultices, applications of a hot paste of wheat bran or flaxseed, covered with flannel, to relieve pain, swelling, or pus draining; or the rectal administration of medicinals. When tissue irritability was decreased, to build up nervous energy, opium and laudanum (opium and saffron, extracted with wine) were used to lessen pain -- though in large doses it was felt they excited rather than relaxed. Purgatives, such as Glaubers salts, Plummer's pills, calomel, ipecac, rhubarb, castor oil, or epsom salts were also prescribed, while stimulants, such as anise, pepper, cinnamon, cloves, dill, sage, ginger, horse radish, nutmeg, horehound, lavendar, marjoram, and spearmint were also used in treatment, as well as rubefacients to irritate and redden the skin. Nourishing broths and liquor were given to dilate the blood vessels. Other medications of the period included epsom salt soaks or quinine-containing bark for ague (fever, recurrent chill, or fits of shivering), and ipecac, blackberry wine, elix asthmaticum (opium, honey, licorice, benzoicacid, camphor, oil of anise, potassium carbonate, and alcohol -- paregoric today) or warm baths and vomits for dysentery. Emetics, such as tartar emetic, ipecac, or warm water and honey, were also popular for the treatment of bilious attacks, jaundice, or digestive problems resulting from bad water or tainted food. For muscular spasms, relaxation, opium, wine (auarts, or even gallons, daily) and ardent spirits were prescribed. To stimulate saliva, as well as to create counter intestinal irritation, mercury in oil was held in the mouth, while camphor or Dover's powder (opium and ipecac) were useful after intestinal symptons were controlled; and to produce perspiration, sweat baths were borrowed from the Indians. And, finally, milk, extracts of dandelions or juniper berries, or lemon juice were advocated as diuretics. Blood-letting, purging, and blistering were used with any of the above. A diet of diluting dreeks, such as barley water, flaxseed tea, or watery gruel, was also often recommended. The body might also be exposed to cool water and air to relieve fever. TopV. Endemic Diseases Smallpox was the principal disease of the 18th century - and the only one with prophylaxis. During the winter of 1777-78, Washington ordered all soldiers and nearby civilians to be pox-proofed. Only one in a thousand failed to recover from the procedure. A healthy donor would supply clear serum from an early vesicle which was opened with a toothpick, and the serum scooped out with a quill; the recipient would then be scratched and the material introduced. This procedure was used until cowpox was discovered in 1798. Another endemic disease was typhus, sometimes known as hospital or jail fever. It was caused by an organism known as a ricketsia, which was introduced into the body by a bite of the body louse. (It was Dr. Rush who suspected that the louse was involved.) The lice were transferred from hospitals to military camps by blankets or clothes. Contributing factors were a lack of cleanliness poor health and diet, fatigue, and the use of linen rather than woolen clothing in the summer. Particularly susceptible were drunks, convalescents, and blacks. The characteristic lesion was petechise, which appeared diffusely. It was considered an excessive stimulation disease, and emetics were the usual therapy. Typhoid fever (or malignant bilious fever, as it was called) was considered the same disease as typhus, but differed in having as symptons signs of diarrhea and rose-colored spots on the chest and abdomen. It was actually spread by contaminated excreta - food, clothing, bedding. Associated with typhoid was dysentery (or diarrhea or flux), which was caused by drinking contaminated water, eating bad food, exposure to cold air, or sleeping in wet clothing. Diphtheria and scarlet fever were also considered the same disease. They were thought to be from "affection of the air", not from contact with other infected people. The treatment for such excessive stimulation was bleeding, as with Washington. Frequently the incisions were made beneath the tongue; a gargle of alum, dissolved in honey and sharp vinegar, could be added. Colds, including influenze (or catarrh), were thought to be caused by close contacts, corrupt air, and a lack of exercise. Yellow fever (or the Great Sickness, American Plague, Barbados Distemper, or Bilious Plague) was a frequent problem in seaport cities and in the southern camps. Its prevention consisted of a number of measures, including heating vinegar in bowls to produce fumes, the oral use of tobacco to produce saliva, with cigars put in the mouths of women and children, carrying handkerchiefs with vinegar or camphor, chewing garlic or putting it into shoes or in a pocket, and the presence of gunpowder. Dengue fever or breakbone fever (also of viral origin and carried by the mosquito aedes aegypti) was characterized by severe back, hip, and leg pain. Malaria, or intermitting fever, was related to bad air, because of its association with "exhalations of marshes". It was distinguished from yellow fever and dengue by periodic onsets of chills and high fever. The therapy for it, quinine bark, was actually on target. Venereal diseases were vague and conveyed "by European soldiers". Their treatment was oral salt peter and sumac roots, or a mixture of salts and turpentine. Consumption was not understood, and was one of the worst diseases at this time. Dental deterioration, as mentioned previously, was extremely common. Rotten teeth were pulled by anyone available. Herbs were used as well. Stress, which has always existed in times of uncertainty, was manifest in 1774-75, when the results of a petition to the King concerning possible reconciliation were awaited. In Philadelphia, a heavy number of cases of "apoplexy" were reported; even one member of Congress, Peyton Randolph, was affected. Nor were suicides uncommon during the colonial period, usually being accomplished by hanging. TopVI. The Medical Department of the American Army After the battle at Bunker Hill and its heavy casualties, the Continental Congress established a "Hospital for the Army" [its term for the medical department] on July 25, 1775. It was to be headed by a Director General, and under him was a chief surgeon, both appointed by the Congress. These two were to be assisted by four surgeons, twenty surgeon's mates, one apothecary, one nurse for every ten men, a clerk to keep accounts, and two storekeepers to serve a total of 20,000 men. In that same year the Congress also established the apothecary unit in the "Hospital" setting. This medical department was inefficient and often ineffective throughout the Revolutionary War for a number of reasons: First, the Continental Congress never established a table of organization for the "Hospital". There were overlapping jurisdictions, and a failure to establish lines of authority and responsibility. State regiments had separate medical services, which were appointed by and under the control of the individual states. New Jersey, for example, in 1775 provided each of its battalions with at least one surgeon, and usually a surgeon's mate. Second, the Congress was too preoccupied with other matters to pay enough attention to the needs of the medical department. Third, rivalries among top medical officers, Congressional politics, and corruption within the service often interfered with the operation of the medical department. Initially, Congress had approved both state-civilian and army-professional medical personnel as a method of democratic checks and balance. The former, with their regimental surgeons, would continue as the home defense and offer support to the Continental army. However, this led to disputes between the Continental army and state militia medical men. And at the top echelon, bitter disputes arose between the first Director General, John Morgan, and his arch-rival, William Shippen, who replaced him later and eventually faced court-martial. Also, some of the lower-level personnel were actually dishonest, and sold medical discharges. Fourth, medical supplies usually were inadequate, and shortages of food and clothing aggravated the problems. Often gross inadequacy prevailed, with a resulting complete absence of medical supplies at the front. Small amounts of supplies were smuggled in from the West Indies or captured from the British, and the French managed to send a few shipments, but it was far from adequate. And fifth, there were too few qualified personnel (surgeons and surgeon's mates) available. General Washington, realizing the inadequacy of the medical personnel, attempted to require surgeons and surgeon's mates to take examinations, but the Congress yielded to states' rights pressure, and nothing happened until much later, when the Congress established a screening board in 1782. Because of the varied abilities of the regimental surgeons, the Director General, John Morgan, issued the following regulations: 1. Dress the wounded by a hill 3000 to 5000 yards to the rear of the battlefield. 2. Regimental surgeons are to be stationed with their militiamen when in a fort or on a defense line, 3. Give emergency care only. In the heat of battle, amputation or any capital operation is best avoided. Duties include: Stop bleeding with lint and compresses, ligatures, or tourniquet. Remove foreign bodies from the wound. Reduce fractured bones. Apply dressings to wounds. If the dressings are too tight, blood flow is decreased and will increase inflammation and excite a fever. If the dressings are too loose, fresh bleeding may occur or set bones may displace. 4. Regimental surgeons and mates are ordered to the general hospital if it becomes over crowded with new casualties. 5. Before battle, check with the regimental officers to carry off the wounded [with] a supply of wheelbarrows, other convenient biers, or whatever other transport available to carry off the wounded. (These orders have a familiar personal ring to recent fast-moving units!) After pressure from General Washington, Congress subordinated the regimental hospitals to the Director General. Washington also ordered the regimental surgeons to make their returns of casualties and supplies to the Director General. There were three types of hospitals: The general hospitals were intensive-care units, established in public or private buildings, and run by the Continental military. They could be single units or a series of buildings, and included homes, barns, huts, churches, and colleges. They were located in relatively stable locations, such as Providence and Newport in Rhode Island; Peekskill, Fishkill, and Albany in New York; Hackensack, Fort Lee, Elizabeth, Amboy, Brunswick, and Trenton in New Jersey; Bethlehem, Bristol, Reading, Lancaster, Manheim, and Philadelphia in Pennsylvania; and Alexandria and Williamsburg (in the Governor's Palace) in Virginia. Flying hospitals were mobile units, being located in a hut or tent, with a few emergency beds and a surgeon's table. They were also manned by Continental personnel. Regimental hospitals were specifically constructed and run by the regimental surgeons. TopVII. The Battle of the Brandywine During the Battle of the Brandywine, the 600 troops that were wounded were dispersed long distances to Philadelphia, Trenton, Princeton, Bethlehem, Ephrata, Lititz, and elsewhere. This was done because of Washington's policy to send casualties ahead of the retreating army, using them as a shield. The wounded, most of them in insufficient clothing, were transported in springless wagons, and by sleds, carts, wheelbarrows, and on stretchers of coats or blankets. TopVIII. The Valley Forge Encampment The encampment of Washington and his troops at Valley Forge from December 19, 1777 to June 19, 1778 -- a period of exactly six months -- is known by most Americans as the time of the greatest suffering during the war, and it may well have been. In December 1777, 3000 troops were sick; by late January 1778, the number reached 6000. By the end of the encampment, of the 10,000 to 11,000 men there, 2500 to 3000, or one-fourth of them, had died of disease, exposure, and privation. Why such a catastrophe? Malnutrition, including scurvy, was the most wide spread problem. The food was said to have been both bad and infrequent. Even though food was available in the interior of Pennsylvania, there were few wagons or teams to haul it. The biggest factors were graft and the inefficiency of the Congress. Agents of the various hospitals actually bid against each other for what food there was, as the medical leaders feuded. On top of this, Dr. Bodo Otto at Yellow Springs recorded that one-half to two-thirds of the wagons were regularly pilfered by the teamsters. Other wagons were captured by the British. The weather, despite the popular impression of persistent snow, to the contrary apparently had little accumulation. However, constant cold rain and sleet prevailed, which directly contributed to such problems as frostbite, chilblains, pneumonia, pleurisy, rheumatism, and tuberculosis. There was only meager knowledge of sanitation. Purification was attempted by wood smoke, sulfur from burnt cartridges (ordered by Washington for each soldiers' hut), burnt tar, and vinegar apread over the floor and furnishings. These steps were thought to thwart "crowd fevers", but such measures were, of course, to no avail. The huts which housed the troops, replicas of which can be viewed today, had floors below ground level, and were cold and damp. The only fuel, green logs, produced a dense smoke. Vermin quickly filled the buildings, as human excreta was frequently deposited from the incapacitated sick. Many died in their huts, and were so quickly buried that adequate records were not made of their deaths. The latrines were rarely used, despite stringent orders -- even to shoot on sight if a man relieved himself elsewhere in the encampment area. In addition, a large number of dead horses and the remains of beef cattle were left unburied about the encampment, which tended to pollute the few sources of potable water. And to compound these problems, disagreements existed among the medical staff with regard to the causes and prevention of camp diseases. Therefore, it was no wonder that these men were prime candidates for yellow fever, typhus, typhoid fever, smallpox; even measles and whooping cough were often fatal. Other conditions noted included scrofula, boils, and other skin infections which sometimes resulted in gangrene. Another skin condition, known as body itch, began between the fingers and spread diffusely, often developing into impetigo. Injuries such as broken bones and ax cuts occurred in the building of the huts and fortifications, and in chopping fire wood. The general hospitals mentioned earlier, as noted, were established in various types of commandeered buildings. At nearby Yellow Springs, however, was erected the only building constructed specifically as a field hospital during the war. It was probably being built in the summer of 1777, 136 feet long and 36 feet wide, with three stories and an attic. The first floor was stone, and rest wood. Samuel Kennedy and Bodo Otto served as its chiefs. It received many of the sick from Valley Forge. Unfortunately, the military hospitals often compounded the problems of the sick and wounded. Benjamin Rush reported, "Hospitals are the sinks of human life in the army. They robbed the U. S. of more citizens than the sword." A soldier had a 2% chance of dying in battle, but when admitted to a crowded army hospital the likelihood of death rose to 25%. Another source reported six out of seven deaths during the war were due to camp illness; another that for every death from wounds there were nine from disease. The dead were buried in grounds adjoining the hospital, in unmarked graves. Not only were the sick and wounded troops vulnerable in the hospital setting; so were the physicians and nurses, particularly in Ephrata and in Bethlehem. In the latter town, nine of eleven surgeons contracted typhus in a four-month period. At Yellow Springs Dr. Samuel Kennedy probably also died of typhus, contracted while working at the hospital. The condition of crowding was universal, and an important factor in the morbidity and mortality rate among the patients. In Bethlehem, where 700 were crowded into a house of the Single Brethren, four-fifths of the two hundred soldiers who died were ill with typhus. The sick were laid on straw in long lines, and because of the scarcity of straw, it was seldom aired or replaced despite General von Steuben's order of frequent airing of bedding and the burning of all straw used by the dead or patients with typhus. Covering for the straw depended upon whatever blankets the patient brought with him, and his bed clothes were whatever clothing he posessed. Sheets were rare. Once in the hospital, the patient had to protect his possessions, as stealing was prevalent. Attempts were made toward cleanliness, but they were usually limited to washing the face and limbs and the combing of hair to try to keep it free from lice. Unfortunately, a constant supply of these creatures was present in the straw and unwashed clothing. Toilets consisted of pails in a corner of the room, and were occasionally emptied. Sometimes metal bedpans were available for the bed-ridden. Because of the overcrowding and the poor conditions, however, the ill were often left in their own filth. Tincture of myrrh and turpentine were used as cleansing agents for wounds. Unfortunately, wounds often were cleaned with plain water which was then drained into a pail or basin and re-used for all the others with wounds in the ward. What better vehicle for the spread of infection! Maggots also frequently appeared in the wounds, but it was soon realized that they helped to remove necrotic material. (In fact, cultured maggots were used until relatively recent times for debriding.) The nutritional aspect was dismal. Food shortages existed, of course, for the hospitalized as well as for the other troops. But the food shortage for the sick was a greater problem, as the especially -needed items were in great demand generally. These included wine, rum, sugar, coffee, tea, milk, molasses, chocolate, mutton, veal, vegetables, rice, fish, and oil. As mentioned earlier, rum, wine, and whiskey were used as stimulants, and in large amounts as a narcotic in surgery. Molasses and sugar provided energy, and aided resistance to infection. Coffee, tea, and chocolate were also used as stimulants. The need for salt was also recognized, but it was unavailable. The invalids were given a liquid diet because it was felt that solid food used up energy needed to fight off the disease. Soups and broths were prepared from Indian corn, barley, rice, fish, and oil. Bread was often combined into the soup or broth to form a mush for more substance. An outstanding method of spreading disease was the custom of feeding the patients from wooden bowls, with pewter or wooden spoons ~ with but one spoon serving the entire ward. TopIX. Physicians' Equipment and Hospital Procedures The physicians' often-depleted medicine chests consisted of bottles of laudanum for relief of pain and diarrhea; cremor tartar and spirits of lavendar to relieve gastric distress; and elixir paregoric for diarrhea, pain, cough, and pausea relief. Three types of medication were prepared: liquids, mixed in copper kettles over fire, and given hot to the patients, usually as purges or emetics; dry powders, prepared with the mortar and pestle; and pills, rolled by the physician. Topical applications to wounds were sprinkled basilicum powder or quinine, but more often whiskey. Cauterization was often employed, especially with bleeding. Wounds might also be packed with lint (scrapings from cotton or linen), and then bandaged and kept damp with water or vinegar. As mentioned earlier, purges, emetics, blisters, poultrices, and flannel compresses tied to plasters and applied to the affected part of the body were used, as well as cupping and the use of leeches. (At least into the early 1940s, leeches were still advertised by an apothecary near the Benjamin Franklin Bridge in Philadelphia.) Surgery usually was in connection with bullet wounds and amputations. Forceps and probes were used for the removal of the bullet and bone from the wound, with amputation often the next step. Until the First World War, when steel-jacketed bullets were introduced, the bullets were made of lead and expanded on impact. Therefore large holes and bone shattering were the result. Amputations were for the most part performed with large curved knives, though later saws were introduced by the British. Anesthesia was provided by the already mentioned alcohol, or by a tobacco juice concoction, and, of course, by the oft-cited "biting the bullet". The patient was restrained -- literally held down -- by attendants, a practice which continued into the latter part of the 19th century. Suturing was performed with a linen thread or sinew, using curved needles like a sailmaker's, the forerunners of today's needles. Other surgery consisted of tooth extraction, done with a corkscrew and hooked metal key. TopX. Hospital Advancements As happens in eyery war, benefits are spun off, and during the Revolution this occurred with hospital care. It was originally the policy that as soon as a patient was mobile, he was generally returned to full duty. It was a policy that was a hindrance both to complete recovery and the proper functioning of his unit. The State of Connecticut in September 1776 became aware that their troops were returning to duty still ill and wounded, and so established small hospitals in every town. These were known as convalescent hospitals, and enabled many soldiers to return fit for full duty more quickly. The disastrous effects of hospitalization during the Valley Forge encampment also led the prominent New Jersey physician, James Tilton, to devise the use of small general hospitals in Moorestown, New Jersey during the winter of 1778-79. Based on a wigwam concept, small log cabins were setup, three in number and in a "U". In the ridge of the roof was a small opening, only four inches wide. A fire was placed in the midst of each cabin, and the air and smoke would circulate about the room before passing through the hole in the roof, thereby providing better ventilation. The floor was the ground, and the feet were turned to the fire. For warm weather, he advocated the use of long tents. The result was a decrease in disease. TopXI. Preventive Care As the war progressed, the army began to recognize the benefits of hygiene and sanitation. This was the major medical advance of the Revolutionary War period. Three publications were instrumental in promoting these benefits: Military Hygiene, published in 1776 by Dr. John Jones; Diseases Incident to the Armies Within the Method of Cure, by Baron von Steuben; and, most especially, "To the Officers in the Army of The United American States: Directions for Preserving the Health of Soldiers, by Dr. Benjamin Rush. Many of the following recommendations were from Dr. Rush's book. For personal care, the hands and feet should be washed once daily, and the entire body two or three times weekly. Stubble was to be removed at least three times weekly (and the soldiers had to pay the barber). Hair was to be thinned, and worn short at the neck, with daily combing and dressing. Since linen hunting shirts absorbed perspiration well, they should be frequently changed. Shoes should be of thick and strong leather, and all seams waterproofed by waxing. (Nevertheless, the troops preferred Indian mocassins, which were considered warmer than the common leather shoes.) In a camp, the tents should be placed on dry spots, well aired and shaded. Areas near marshes and bodies of water should be avoided, as should also be the sun. Fire, wood smoke, burning sulfur, and exploding gunpowder were felt to preserve and restore the purity of the air. Straw should be frequently changed. Blankets were to be aired in the sun. Bedding was to be raised off the ground. There was to be no elimination about the camp except in privies. If flux or diarrhea occurred, deep pits were to be dug, with a thick layer of earth to cover deposits. The privies were to be placed either in front of or to the rear of the camp, depending on the direction of the prevailing winds. For diet and victuals, chiefly vegetables and fresh fruit were advocated. Bread was to be well baked, and of pure flour. Cooking vessels were to be carefully washed after using, a necessity proven in every military organization since then. Drinking water must be pure; river water from near the banks should be avoided. Water purity was to be checked with a few drops of oleum tartari -- if it was pure, only a small cloud would appear in the water. When impure water was suspected, six ounces of vinegar were to be added to three quarts of water. TopXII. Conclusions In conclusion, several positive effects occurred. The principles of sanitation and hygiene began to be recognized. Steps in disease control were initiated. The importance of smallpox vaccination was established. A policy for battlefield treatment of the wounded and their evacuation was recognized. And initial efforts at structuring a military medical department were made. But it was just a beginning, and significant advances in surgery and anesthesia, as well as other phases of care for the sick and wounded, were still many years in the future. TopBibliography Beck, James B. Medicine in The American Colonies. Horn & Wallace, 1966 Brinton, Robert. Notes re Yellow Springs Hospital in the Revolutionary War. Burkhart, Larry L. The Good Fight: Medicine in Colonial Pennsylvania,1681-1765. University of Michigan Films, 1982 Cowen, David L. Medicine in the Revolutionary New Jersey. New Jersey Historical Society Commission, 1975 Moorestown Memorial Hospital. Medicine and Surgery During the American Revolution. O'Connor, Robin. American Hospitals: The First 200 Years. Hospitals [Journal of the American Hospital Association! January 1, 1976 Valley Forge National Park. Valley Forge Are Folk Cultural Study, Valley Forge Research Project Report. Wilbur, C. Keith. Revolutionary Medicine 1700-1800. Globe Pequot Press, 1980 TopAcknowledgements Bob Goshorn steered me into this project -- which I have thoroughly enjoyed -- and recommended several resources. Ruth Vanderslice, a friend who volunteers at the Valley Forge National Park Library, not only cheerfully dug out much of the material, but also photographed it and provided me with other publications. Guy Ghisu, photographer and projectionist of the Delaware County Memorial Hospital, prepared the slides -- which wasn't easy. And my wife Beverly; she bore other burdens and provided me with the time for this project. I might add that this is a belated acknowledgement for her support in other ventures too. 1. At that time it was thought the body had twelve, rather than six, quarts of blood. On his deathbed, George Washington had nine pints of blood drawn in twenty-four hours!
|